Is it safe to go to the dentist?
We asked experts about dental office safety protocols amid the pandemic
If the coronavirus is spread through breathing without a mask in close proximity to others, then one might think that sitting with one’s mouth agape for hours while a hygienist fiddles right next to you seems like a risky proposition. Indeed, unlike other health care visits, dentistry requires the removal of one’s mask for long periods. That has many Americans delaying or avoiding dental care, out of fear of transmission.\
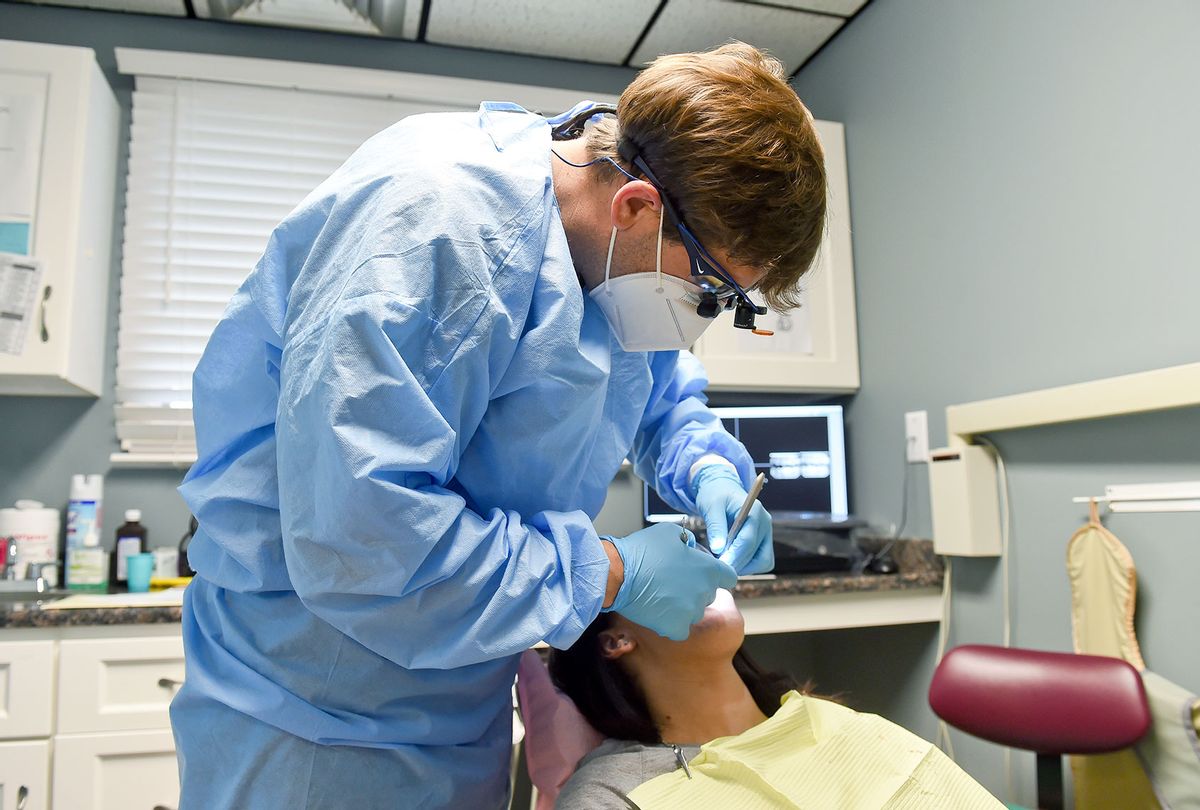
But don’t delay your dentist visit just yet. Dentists and health care experts say that despite what it might appear, a dentists’ office visit is actually a paragon of pandemic safety.
“It’s very safe to go to the dentist, and it’s been really safe since dental offices reopened back in May,” said Dr. Kami Hoss, D.D.S., who sits on the Board at the UCLA School of Dentistry and is the CEO of The Super Dentists in California. “Dentists are infection control experts.”
Dr. Hoss said that dentists have been hyper-aware of disease transmission and how to avoid it for decades. “This goes back to the 1980s, when I was going to dental school when we had to deal with the HIV AIDS crisis,” Hoss said. “Since then we have implemented many processes, technologies, and protocols to make sure that we keep our patients, employees and doctors safe.”
Despite being considered a “high-risk” profession, in part due to the close proximity between dentists and patients, a report published by The Journal of the American Dental Association (ADA) found that less than one percent of 2,200 dentists surveyed last June had COVID-19. Professionals in the industry believe the low rate is a result of the industry adding an extra layer of protection to their already-stringent sanitation standards.
Dr. Matt Messina, an ADA spokesperson, told Salon over the phone — in-between patients — that it’s “absolutely” safe to go to the dentist right now. He remarked that there’s been no dentist to patient transmission that the ADA is aware of, and that the fact that less than 1 percent of dentists surveyed in June contracted COVID-19 means the industry has “a pretty amazing record.”
“And that’s dentists that have come down with COVID, and that includes from any source,” Dr Messina said of the statistic.
But of course, like mostly everything else, going to the dentist right now looks a bit different than it did pre-pandemic. You don’t get the coffee or tea in the waiting room, or likely any leisure time to read magazines before getting your teeth cleaned, like you did before. Some offices have omitted the waiting room entirely, opting instead to have patients wait in their car for a call when they’re ready to be seen. And prior to your appointment, you can expect to be virtually screened for possibly being exposed to COVID-19 and any potential symptoms— like Dr. Hoss does in California.
“We’ve implemented a thorough phone screening going through all the questions — if you have a fever, if you’ve been around COVID, we start from there,” Dr. Hoss said. “We only allow healthy people inside; that screening includes patients, but it also includes our staff and our doctors, every single morning before they’re allowed to be entering the offices.”
In addition to pre-appointment screening, dentists will look a little more protected too.
“Most patients will see, maybe the addition of face fields, more of a barrier gown type of arrangement, we look a hair more surgical than we have in the past,” Dr. Messina said. “Dental offices have used gowns, goggles, face shields, masks, even from before so luckily the average patient won’t notice a big difference.”
The Centers for Disease Control and Prevention (CDC) has listed exhaustive measures for the dental industry to follow. The federal agency also advises that dentals offices prioritize dental services and overall care based on the personal protective equipment available and how many COVID-19 cases are in one’s local community. The risk of COVID-19 transmission is often weighed against the risk of not taking care of your oral health, which both dentists emphasized to Salon is very important.
“It is absolutely necessary to take care of your oral health, especially during a health pandemic,” Dr. Hoss said. “Why? Because general health starts in your mouth, oral health impacts every part of our health, including the health of pregnancy — it’s connected to many many systemic diseases, including lung health.” Indeed, the coronavirus can become deadly when it infects enough cells in the lungs.
But what about the metal tools that go in your mouth during a cleaning— the ones that are usually in someone’s mouth before yours? Dr. Hoss said a lot more “disposable items” are being used, but those “metal pieces” are being sterilized just like before. And that’s because the coronavirus is actually quite easy to kill (hence, the large public-health emphasis on washing hands and countertops).
“This particular virus is actually very sensitive to soap, even,” Dr. Hoss said. “For our sterilization process, there does not need to be dramatic changes to it. So yes we do use a lot more disposable items as much as possible, but anything that we can’t and we have to use it between patients, it’s fully sterilized and fully cleaned and it’s completely safe to be used between patients.”
